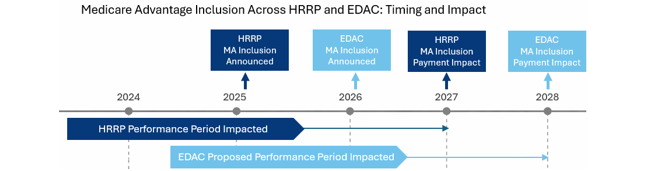
The FY 2027 IPPS Proposed Rule, released by CMS on April 10, further expands the patient population included in post-discharge outcome measures. Specifically, it proposes adding Medicare Advantage patients to the Excess Days in Acute Care (EDAC) measure.
This follows the FY 2027 IPPS Final Rule, which confirms that hospital readmission penalties will include Medicare Advantage patients. Together, these changes significantly alter how successful care transitions are measured and increase pressure on downstream providers to ensure safe transitions within 30 days of discharge.
Signs that Medicare Advantage Inclusion Will Continue to Expand
While the EDAC change is a hospital-specific update, CMS’s rationale clearly extends beyond the acute care setting to effectively assess care transitions and avoidable acute utilization among a large population of Medicare beneficiaries.
The proposed rule notes that “since the initial adoption of these measures, the proportion of Medicare Advantage beneficiaries has increased from 35 percent of the Medicare population to over 50 percent.” CMS also emphasizes that “capturing care transition outcomes for all Medicare beneficiaries for these acute conditions continues to be a high priority.”
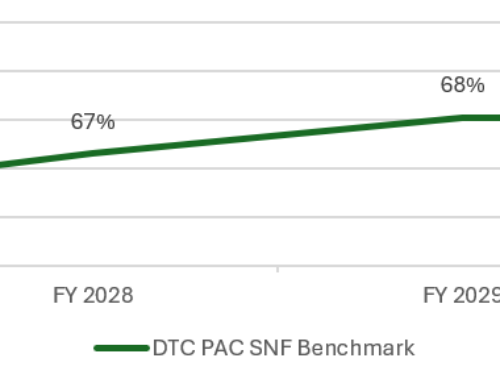
Although certain SNF post-discharge outcome measures, such as the rate of successful return to home or community, still exclude Medicare Advantage patients, this may change. CMS has signaled a desire to align quality reporting with a broader all-payer model.
A recent example is the FY 2027 SNF PPS Proposed Rule, which proposes requiring SNFs to submit Minimum Data Set data for all residents, regardless of payer source, including Medicare Advantage, Medicaid, and private pay.
How EDAC Measures Post-Discharge Outcomes
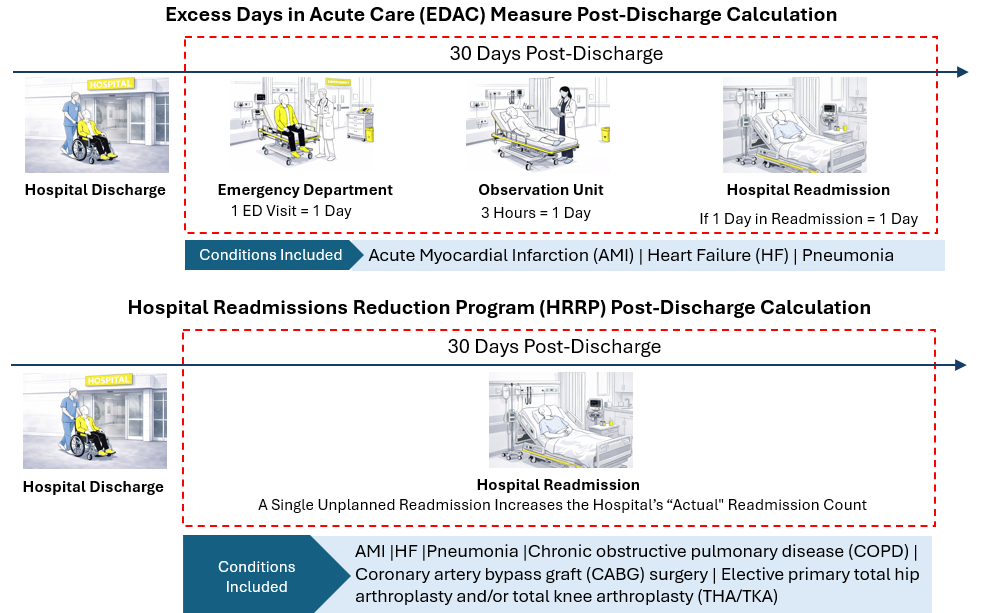
EDAC is an outcome-based quality measure that tracks the total number of days a patient spends in an emergency department, under observation, or in an unplanned readmission within 30 days of discharge. This total is compared to the expected number of days for similar patients.
EDAC differs from the Hospital Readmissions Reduction Program (HRRP), which measures only whether a patient is readmitted. Both measures use a 30-day window, but EDAC focuses on utilization, while HRRP focuses on readmission occurrence.
EDAC currently applies to patients with acute myocardial infarction, heart failure, and pneumonia. While HRRP can impose penalties of up to 3 percent of total Medicare inpatient revenue, EDAC contributes to a hospital’s Overall Hospital Quality Star Rating.
What Skilled Nursing Can Do in Anticipation of Similar Changes to EDAC
If CMS finalizes the inclusion of Medicare Advantage patients in EDAC, hospitals will face greater scrutiny across all payer types. This will likely extend to their post-acute partners.
Because the policy would apply to the July 1, 2024 performance period, evaluations may reflect past performance. Skilled nursing providers should be prepared to demonstrate strong outcomes for all patients, not just those in traditional Medicare.
Emphasizing specialty programs and certifications, such as American Heart Association Heart Failure Certification, can help differentiate providers. In addition, providers should clearly demonstrate how they support patients discharged before the 30-day window, as hospitals remain accountable for outcomes during that period.